The Epidemic That Turned People into Living Statues
Between 1917 and 1927, a mysterious disease put over a million people to sleep. Some of them didn't wake up for forty years. We still don't know what caused it.
Key Facts
- Over **1 million people** were infected worldwide between 1917 and 1927
- Approximately **500,000 died**; a third of survivors were left permanently disabled
- Some patients remained in catatonic states for **over 40 years** with their minds still active
- The cause has **never been identified** despite over a century of research
- The last known survivor, Philip Leather, died in **2002** at age 82
The Winter It Began
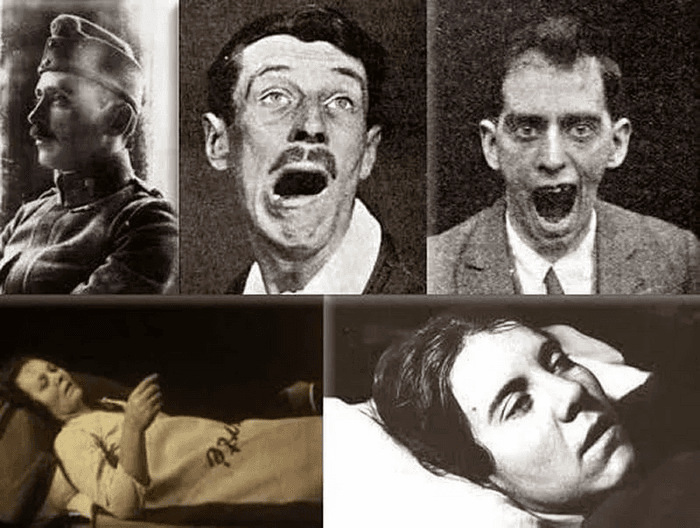
During the winter of 1916-1917, in the middle of a world war that was already killing millions, a Viennese neurologist named Constantin von Economo began seeing patients with symptoms that didn't match anything in his medical training. They came in complaining of headaches, malaise, and low-grade fevers — nothing unusual for wartime Vienna. But then something strange happened. They fell asleep. Not ordinary sleep — a profound, unreachable unconsciousness that could last for days, weeks, or months. Some patients could be briefly roused but would immediately drift back under, as if pulled by an irresistible gravitational force.
Others went the opposite direction. Instead of sleeping, they couldn't stop moving — manic, twitching, insomniac, their bodies jerking with involuntary motions they couldn't control. Still others became rigid, their muscles locking them into position like mannequins, conscious but unable to move or speak. Three wildly different presentations, all caused by the same unknown illness attacking the brain.
Von Economo published his findings in 1917, naming the condition encephalitis lethargica — literally "inflammation of the brain that makes you drowsy." Within months, it was everywhere.
The Man Who Named It

Von Economo himself was a remarkable figure. Born in 1876 to a wealthy Greek family in what is now Romania, he initially studied mechanical engineering at the Vienna Polytechnic before switching to medicine. He earned the title of Freiherr (Baron) in 1906. He was a passionate aviator who obtained Austria's first international pilot's diploma in 1912 and served as president of the Austrian Aero-Club for sixteen years. He married Princess Karoline von Schönburg-Hartenstein. In another era, he might have been remembered primarily as an eccentric aristocrat who flew planes and mapped the brain's cortex.
Instead, history remembers him for a disease he saw while treating head injuries during World War I — a disease that would infect over a million people, kill roughly half a million of them, and then vanish as mysteriously as it appeared, leaving behind thousands of people trapped inside their own frozen bodies.
A Pandemic Inside a Pandemic
The timing of encephalitis lethargica has haunted researchers for a century. The epidemic overlapped almost perfectly with the 1918 influenza pandemic — the deadliest plague in modern history. For decades, the obvious assumption was that the sleeping sickness was somehow caused by, or related to, the flu. It was a reasonable hypothesis. Both were neurological in some of their effects. Both swept the globe at roughly the same time. The simplest explanation was that the flu virus was attacking the brain in some patients, triggering the encephalitic symptoms.
But the data never quite fit. The outbreaks didn't track geographically — cities hit hardest by the flu weren't necessarily the ones with the most sleeping sickness cases. And when modern researchers examined preserved brain tissue from encephalitis lethargica patients using techniques unavailable in the 1920s, they found no trace of influenza virus. None.
The epidemic peaked between October 1918 and January 1919 — right at the height of the influenza catastrophe — then surged again across the United States between 1920 and 1924. By 1927, it had essentially vanished. New cases became extraordinarily rare. In the 85 years since the epidemic ended, only about 80 cases have been documented worldwide. The disease didn't evolve or get treated — it simply stopped.
The Three Faces of the Illness
Von Economo identified three primary forms of the disease, and each was its own particular nightmare.
The somnolent-ophthalmoplegic form was the most common and the one that gave the disease its name. Patients fell into a deep, prolonged sleep from which they could sometimes be partially awakened. Their eye muscles became paralyzed, giving them a distinctive fixed stare. Some slept for weeks. Others slept for months, wasting away on hospital beds while their families waited for them to wake up.
The hyperkinetic form was the opposite: patients became manic, sleepless, and physically agitated, their bodies wracked by involuntary movements and twitches. They couldn't rest, couldn't be still, couldn't stop the electrical storm in their brains from translating into constant, exhausting motion.
The amyostatic-akinetic form was perhaps the cruelest. Patients became rigid — locked in place, fully conscious, but unable to move, speak, or communicate. Their reflexes still worked. Their minds were still intact. They were awake and aware inside bodies that had become prisons. Some would remain in this state for decades.
Roughly a third of patients died during the acute phase. A third recovered without lasting effects. And a third — hundreds of thousands of people — entered the chronic phase: postencephalitic parkinsonism, a condition that could develop one to five years after the initial illness and then persist for the rest of their lives.
Frozen for Forty Years
By the 1930s and 1940s, hospitals and institutions across Europe and America housed thousands of people with postencephalitic parkinsonism. Many had contracted the disease as children or young adults. Now they sat in wheelchairs or lay in beds, rigid, silent, staring. Nurses could pose their limbs like dolls, and the limbs would stay where placed. They couldn't initiate movement, couldn't start a sentence, couldn't reach for a glass of water — but if a ball was thrown to them, some could catch it. If music played, some could dance. The automatic motor pathways still worked; it was only voluntary movement that had been stolen.
Their minds, as far as anyone could tell, remained intact. During rare moments of lucidity — sometimes triggered by fever, emotional shock, or simply unpredictable fluctuations in their disease — patients could speak, move, and interact normally, revealing minds that had been fully aware and thinking for years or decades inside unresponsive bodies. Then the window would close, and they'd freeze again.
The last known survivor of the original epidemic, Philip Leather, died in 2002 at age 82. He had been institutionalized since childhood — over seven decades spent locked inside a body that wouldn't obey him, in a world that had largely forgotten the epidemic that put him there.
The Awakenings
In 1966, a young neurologist named Oliver Sacks arrived at Beth Abraham Hospital in the Bronx. He found a ward full of these patients — survivors of the 1920s epidemic, now middle-aged or elderly, sitting in the postures they'd been frozen in for decades. Sacks was fascinated and moved by them. He spent hours observing, talking to them during their rare lucid moments, documenting the extraordinary complexity of their condition.
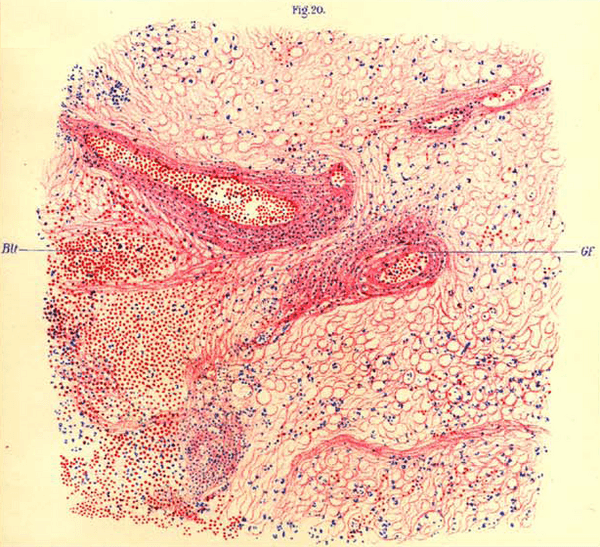
In the late 1960s, a new drug called L-DOPA was showing promise for Parkinson's disease. The connection was logical: both Parkinson's and postencephalitic parkinsonism involve damage to the substantia nigra, the brain region that produces dopamine. If L-DOPA could help Parkinson's patients by flooding the brain with the dopamine precursor it could no longer make for itself, maybe it could help these patients too.
Sacks decided to try. And what happened was, by his own account, one of the most extraordinary things he ever witnessed in medicine.
The patients woke up.
People who hadn't moved voluntarily in twenty, thirty, forty years suddenly stood up, walked, talked, laughed. They recognized family members. They asked what year it was. They were the same people they'd been before the disease — just transported decades into the future, into a world that had changed beyond recognition while they sat motionless in a hospital ward.
Sacks documented these experiences in his 1973 book Awakenings, which was later adapted into a 1990 film starring Robin Williams as Sacks and Robert De Niro as one of his patients. The book remains one of the most remarkable documents in neurological literature — a work of science that reads like tragedy.
The Mystery That Won't Die
More than a century after the epidemic began, we still don't know what caused encephalitis lethargica. This isn't for lack of trying. The disease has been studied by some of the best minds in neurology and infectious disease, using every modern tool available, and the answer remains frustratingly out of reach.
The leading theories have shifted over time. The influenza hypothesis dominated for decades but has largely fallen out of favor — the epidemiological data doesn't support it, and no flu virus has ever been found in preserved brain tissue. A 2012 study examining preserved samples identified virus-like particles resembling coxsackie B4 virus (an enterovirus), which represents the most compelling evidence for a viral cause. Enteroviruses are known to cause neurological disease, and the finding was intriguing — but it hasn't been replicated.
The most provocative recent theory involves autoimmunity. Researchers have proposed that the disease might have been triggered by a streptococcal infection (like strep throat) that caused the body's immune system to attack its own brain through a process called molecular mimicry — the immune system mistakes brain proteins for bacterial proteins and destroys them. This mechanism is well-documented in other conditions, particularly in children.
A 2024 study from UCL found that almost half of the patients originally diagnosed with encephalitis lethargica might have had autoimmune encephalitis — specifically, a type involving antibodies against NMDA receptors (the same receptors involved in memory formation). But it didn't quite match any of the autoimmune encephalitis types we recognize today, suggesting it might be something we haven't fully characterized yet.
The uncomfortable truth is that we may never know for certain. The epidemic ended nearly a century ago. The patients are gone. The preserved tissue samples are limited. And whatever pathogen or trigger caused it — whether virus, bacterium, environmental toxin, or autoimmune cascade — may have changed, evolved, or simply disappeared.
Could It Happen Again?
This is the question that keeps researchers working on the problem. If we don't know what caused the epidemic, we can't know whether the conditions that produced it might recur. Sporadic cases of what appears to be encephalitis lethargica still occur — roughly 80 have been documented since the epidemic ended — suggesting that whatever mechanism triggers the disease hasn't entirely vanished from the world.
The COVID-19 pandemic added urgency to this question. Like the 1918 flu, COVID-19 is a respiratory virus capable of causing neurological complications. Some researchers have drawn parallels between long COVID's neurological symptoms and the aftereffects of encephalitis lethargica, though the comparison remains speculative. If encephalitis lethargica was indeed triggered by an autoimmune response to a common infection, then any new pandemic could theoretically produce a similar wave of cases — different virus, same devastating outcome.
Understanding what happened in 1917 isn't just historical curiosity. It's epidemiological prevention.
The Deeper Resonance
There's something profoundly unsettling about encephalitis lethargica that goes beyond the medical mystery. These were people who were fully conscious inside unresponsive bodies for decades. They could hear, could think, could feel time passing — but couldn't reach the world around them. When the L-DOPA briefly unlocked them, they didn't emerge confused or diminished. They emerged as themselves, unchanged, asking about people and places from decades earlier, as if no time had passed at all.
What does that say about consciousness? About identity? About where "you" actually reside when your body stops cooperating? Oliver Sacks spent the rest of his career grappling with these questions, and he never fully answered them. Neither has anyone else.
Meanwhile, somewhere in the intersection of virology, immunology, and neuroscience, the cause of the sleeping sickness waits to be found — a medical mystery from the age of horse-drawn ambulances that still defeats every modern tool we throw at it. Sometimes the past doesn't stay past.